FAQ

Frequently Asked Questions
Why are preventive services important?
Preventive services can find health problems early when treatment works best and can keep you from getting certain diseases or illnesses. Medicare pays for many preventive services to keep you healthy. Talk with your doctor or health care provider to find out what tests you need and how often you need them to stay healthy.
How much does Medicare Part A (Hospital Insurance) cost?
Most beneficiaries do not pay a monthly premium for Medicare Part A coverage if they or their spouse paid Medicare taxes while working. In fact, according CMS, approximately 99% of Medicare beneficiaries do not have to pay Medicare premiums on Part A because they have over 10 years (or 40 quarters) of Medicare-covered employment. For the small percentage of people who do have to pay Medicare premiums, the amount per month depends on the number of quarters of Medicare-covered employment the person (or his/her spouse) has:
- People with 30 to 39 quarters of Medicare-covered employment pay a monthly premium of $248 in 2012.
- Those with less than 30 quarters of Medicare-covered employment and who are not eligible for free or reduced Medicare premiums for any other reason pay a monthly premium of $451 in 2012.
- Premium amounts may change for the 2013. CMS generally announces rate changes for the following calendar year around the middle of October each year.
How much does Medicare Part B (Doctor Insurance) cost?
The Medicare Part B premium is based on annual income and cost of coverage. The standard premium ($99.90 for 2012)—the premium for most enrollees—applies to those with annual household incomes that do not exceed a set threshold amount ($85,000 in 2012 for single filers or married couples who file separately and $170,000 for couples who file jointly). The premium is set each year at a level calculated to pay for 25 percent of the average cost of coverage. For 2013, the projected standard Part B premium is $109.10, which is a 9% increase over 2012.*
Although most beneficiaries pay the standard rate, there are three provisions that alter the premium rate for certain Part B enrollees:
Although most beneficiaries pay the standard rate, there are three provisions that alter the premium rate for certain Part B enrollees:
- There is a premium surcharge for those beneficiaries who enroll after their initial enrollment period.
- A "hold-harmless" provision can lower the premium rate for those who have their premiums deducted from their Social Security check. This provision limits the dollar increase in the Part B premium to the dollar increase in the person's Social Security benefit.
- There are higher "income-related" premiums for those whose annual income exceeds the threshold amount. These premiums are calculated to pay for 35, 50, 65, or 80 percent of the average cost of coverage, depending on income level.
What are the Medicare Deductibles for 2012?
Medicare Part A Deductibles
Medicare Part A pays all covered hospital, skilled nursing facility, and home health care services for each benefit period except for the deductible. For 2012, the deductible is $1,156 for any hospital stay 60 days or less. For any hospital stay lasting longer than 60 days, a Medicare copayment will apply:
For people on Medicare who receive care in a skilled nursing facility, Medicare will cover days 1 through 20 in full. There is a copayment of $144.50 per day for days 21 through 100, and no coverage after day 100 in a benefit period.
Medicare Part B Deductible
Medicare Part B includes a yearly deductible of $140 in 2012. This deductible will be applied to health care costs that involve physician services, outpatient hospital services, certain home health services, and durable medical equipment. Once the deductible is met, you will be required to pay only 20% of the Medicare-approved amount charged by providers for your health care services. Because of the new health care law, many preventive services are also provided at no cost to you. These free benefits are not subject to a deductible.
Medicare Part D Deductible
The annual deductible for the standard Medicare Part D benefit will be $325 in 2013, an increase of just $5 from the 2012 deductible. No Medicare drug plan may have a deductible more than $325 in 2013, although some plans may have a lower deductible or no deductible at all.
Medicare Part A pays all covered hospital, skilled nursing facility, and home health care services for each benefit period except for the deductible. For 2012, the deductible is $1,156 for any hospital stay 60 days or less. For any hospital stay lasting longer than 60 days, a Medicare copayment will apply:
- 61 to 90 days: $283 per day
- 91 to 150 days: $578 per day
- More than 150 days within a single benefit period: Full cost
For people on Medicare who receive care in a skilled nursing facility, Medicare will cover days 1 through 20 in full. There is a copayment of $144.50 per day for days 21 through 100, and no coverage after day 100 in a benefit period.
Medicare Part B Deductible
Medicare Part B includes a yearly deductible of $140 in 2012. This deductible will be applied to health care costs that involve physician services, outpatient hospital services, certain home health services, and durable medical equipment. Once the deductible is met, you will be required to pay only 20% of the Medicare-approved amount charged by providers for your health care services. Because of the new health care law, many preventive services are also provided at no cost to you. These free benefits are not subject to a deductible.
Medicare Part D Deductible
The annual deductible for the standard Medicare Part D benefit will be $325 in 2013, an increase of just $5 from the 2012 deductible. No Medicare drug plan may have a deductible more than $325 in 2013, although some plans may have a lower deductible or no deductible at all.
What is Medicare Advantage and what is the cost?
Medicare Advantage Plans, also called Medicare Part C (combines A, B and may include D into an HMO or a PPO with a private insurer). Medicare Part C governs the way Medicare benefits are provided by companies that contract with the Medicare program. Someone with Medicare who enrolls in a Medicare Advantage plan generally gets all of their medical services through that plan. Health Maintenance Organizations (HMO's), Preferred Provider Organizations (PPOs) and Private Fees For Service (PFFS) contract with Medicare to provide Medicare benefits in a managed care setting, that since 2006 includes the new Medicare Part D benefit in all but a few HMOs. People enrolling in one of those plans without Part D benefits would need to buy separate coverage for that benefit. You must pay the Part B premium in order to qualify for a Medicare Advantage Plan. The cost or "premium" for Medicare Advantage plans may vary from $0 to $100 or more per month depending on the area you live in.
What is Medicare Part D?
Medicare Part D is prescription drug coverage (a Stand-Alone Plan with a private insurer) that offers some help with prescription drugs. The coverage is voluntary and the monthly premium varies depending on how much coverage you have. Part D can also be provided in a Medicare Part C plan (Medicare Advantage Plan).
How much does Medicare Part D cost?
Medicare Part D Premiums vary. The monthly Medicare Part D base premium is set to pay 25.5 percent of the cost of standard coverage, based on bids submitted annually by Part D plans. CMS releases the Medicare Part D base premium in early August each year. Actual premiums are based on this set premium, but can vary greatly by plans and regions.
If you decide not to join a Medicare Prescription Drug Plan when you're first eligible, and you don't have other creditable prescription drug coverage, or you don't get Extra Help, you'll likely pay a late enrollment penalty.
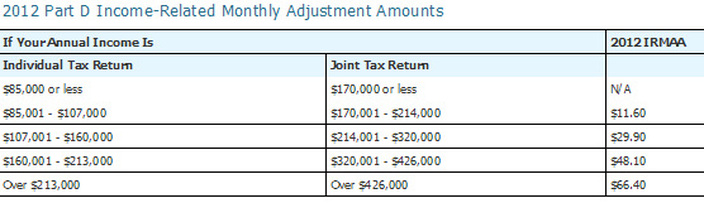
As of 2011, beneficiaries with higher incomes must pay a premium adjustment based on their income. This premium adjustment is called the Income-Related Monthly Adjustment Amount (IRMAA), and is automatically deducted from the Social Security benefit. For 2012 the adjustments are:
If you decide not to join a Medicare Prescription Drug Plan when you're first eligible, and you don't have other creditable prescription drug coverage, or you don't get Extra Help, you'll likely pay a late enrollment penalty.
As of 2011, beneficiaries with higher incomes must pay a premium adjustment based on their income. This premium adjustment is called the Income-Related Monthly Adjustment Amount (IRMAA), and is automatically deducted from the Social Security benefit. For 2012 the adjustments are:
What is Medigap?
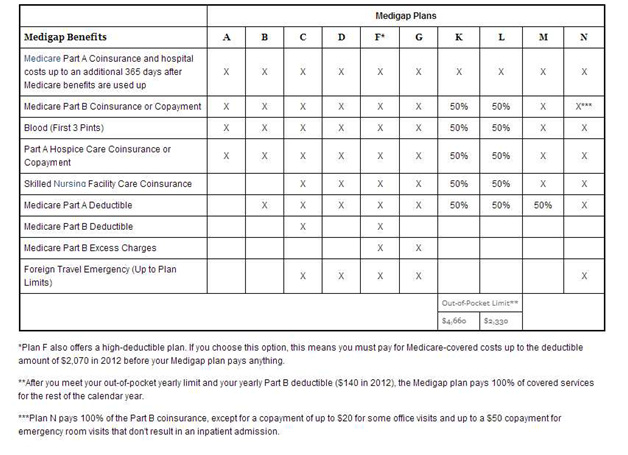
Medigap, also called "supplemental insurance, " is private that provides additional insurance coverage. Generally, when you buy a Medigap policy you must have Medicare Part A and Part B. You will have to pay the monthly Medicare Part B premium. In addition, you will have to pay a premium to the Medigap insurance company. A Medigap policy is health insurance sold by private insurance companies to fill the “gaps” in Original Medicare Plan coverage. Medigap policies help pay some of the health care costs that the Original Medicare Plan doesn’t cover. If you are in the Original Medicare Plan and have a Medigap policy, then Medicare and your Medigap policy will pay both their shares of covered health care costs. Medigap policies can be costly, but useful policies, and can be avoided if you use a Medicare Advantage Plan (above). Please see the chart below that list Medigap Plans A-N and benefit coverges.